The Myth of Patient Fraud
The structure of healthcare in France means fraud by health professionals is widespread, as a recent case has exposed.


The Myth of Patient Fraud
28th April 2026
The structure of healthcare in France means fraud by health professionals is widespread, as a recent case has exposed.
Last month the French legal authorities dismantled a €58 million healthcare fraud network.
The investigation, led by the Paris prosecutor’s office, uncovered a sophisticated system centred on 18 healthcare centres, many of them dental clinics.
These structures were used to generate mass billing for fictitious treatments, frequently under stolen or fabricated identities. Some patients had never set foot in the centres; others did not exist. In one case, procedures were billed under the name of a dentist who had been dead for years.
Although the dominant narrative of welfare fraud often focuses on patients, the case has highlighted the extent of organised health care fraud and the role of health professionals in the process.
According to a recent report from the French health authority, although patients account for more than half of detected fraud cases (mainly sickness benefits), they represent only 16% of financial losses. By contrast, healthcare professionals and related actors account for roughly 28% of cases but nearly 73% of the amounts involved.
Fraud by health professionals detected last year was over €500 million, as detailed on the graphic below.
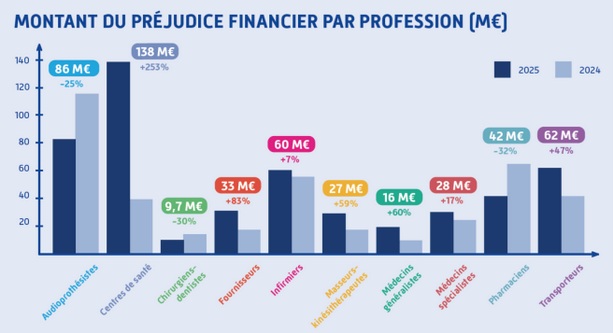
Estimates indicate that real fraud linked to healthcare providers may exceed €1 billion per year.
In absolute terms, the estimated level of fraud by patients, professionals and organised criminal gangs exceeded €2.1 million in 2024.
The French national auditor the Cour des comptes estimates overall healthcare fraud at between €4 billion and €4.5 billion annually.
The organisation of the French healthcare system plays a central role in enabling these practices. The reimbursement model relies heavily on self-declaration by practitioners who submit claims directly to the insurance system.
The billing system itself is highly complex, involving detailed procedure codes, variable tariffs, and multiple reimbursement schemes. This complexity creates opportunities for manipulation and makes it difficult to distinguish between legitimate billing and fraud.
The health authority state that common fraudulent practices identified in their investigations include:
billing for procedures that were never performed;
overcoding, or charging for more expensive acts than ;those delivered;
duplicating medical acts;
inflating the number or frequency of treatments;
misuse or theft of patient identities.
Some of the largest fraud amounts now originate from individuals or networks that are not traditional healthcare providers but exploit healthcare structures for financial purposes. For example, audiology-related fraud has been estimated at €86 million, while fraud involving medical transport providers reached €62 million.
Multi-site healthcare centres have become a central feature in many large fraud cases. Their number has increased significantly over the past decade, particularly in dentistry, ophthalmology, and audiology.
The centres often operate under third-party payment systems, meaning patients do not pay upfront. As a result, patients may be less likely to monitor the care billed in their name.
The centres do not operate like traditional doctor’s surgeries (cabinets médicaux). Ownership of the centres and medical practice are often separated. They are also sometimes staffed by ‘psuedo’ professionals, rather than fully qualified medical staff. The government has recently introduced new controls on those permitted to set up such centres.
In July 2023, health authorities took the exceptional step of removing 13 ophthalmology centres operated by Alliance Vision from the reimbursement system due to fictitious billing and rule violations. Eight individuals have since been indicted on charges including organised fraud, money laundering, and illegal medical practice.
Last year, 23 medical centres were removed from the health system, after 30 in 2024 and 21 in 2023.
Related Reading:
You just read an issue of France Insider. You can also browse the full archives of this newsletter.